Outbreak Response:
Responding to cVDPVs
In 2017, the number of circulating vaccine-derived polio cases (cVDPVs) surpassed the number of wild polio cases globally for the first time. The majority of these cases were in Africa. Since 2001, the African region has reported 894 cVDPV cases, and as of August 2020, 16 countries are currently facing cVDPV outbreaks.
Background on cVDPVs
In rare instances, when not enough children are vaccinated with the oral polio vaccine (OPV), the weakened virus in the vaccine can pass among under-immunized populations and, over time, change to a form that can cause paralysis. This is known as cVDPV. Low immunization rates in Africa mean cVDPVs are a threat in the region.
Though cVDPVs are a challenge, OPV is still vital for combating polio and is responsible for bringing the world to the brink of eradication. First, it protects the entire community: when a child vaccinated with OPV excretes the vaccine virus into the environment, others in close contact can receive protection through contaminated food or water – what is known as “passive vaccination.” Second, OPV is inexpensive and the drops are easy to administer in mass immunization campaigns. Thanks to OPV and eradication efforts globally, 18 million people are walking today who would have otherwise been paralysed by polio. Every year, an additional 650,000 cases of paralysis are averted around the world because of the widespread use of polio vaccine.
Vaccination teams in Monrovia, Liberia, go door-to-door during a four-day national integrated polio campaign to deliver polio vaccines, vitamin A and deworming tablets to 900,000 children, 2015 ©️ UNICEF
Due to ongoing outbreaks globally, the Global Polio Eradication Initiative (GPEI) launched a comprehensive new strategy for 2020-21 to control cVDPVs. The first part of the strategy’s three-pronged approach involves putting together a rapid response team (RRT). In Africa, the team was formed in September 2019, coordinated from the WHO Regional Office for Africa (WHO AFRO) in Brazzaville and composed of 20 experts drawn from the GPEI’s core partners, including WHO, UNICEF, the U.S. Centres for Disease Control and Prevention (CDC), and the Bill & Melinda Gates Foundation.
People from the RRT are the first responders: every time a new cVDPV outbreak is confirmed or even suspected in the African region, the team is dispatched to the country within 72 hours. First, they investigate reported cases and carry out a risk assessment. Thereafter, the team establishes coordination mechanisms, develops a six-month outbreak response plan and budget, and prepares for the initial outbreak response campaign.
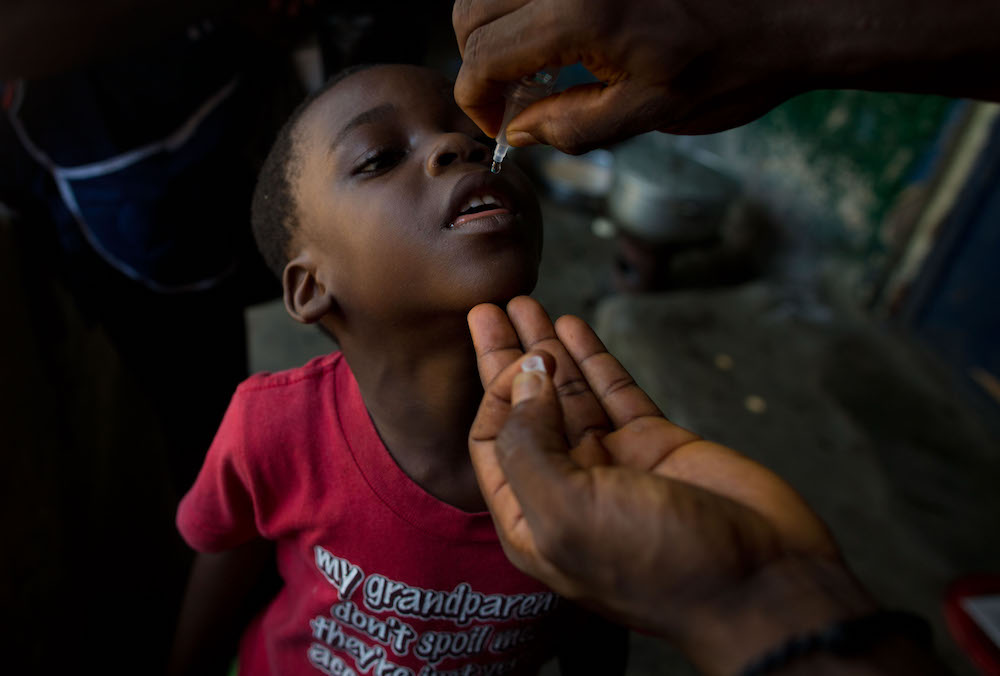

A girl receives a polio vaccine (left) and a girl shows her pinky finger which is painted after receiving the polio vaccine during a four-day national integrated polio campaign to deliver polio vaccines, vitamin A and deworming tablets to 900,000 children, 2015. ©️ UNICEF



Rapid Response Teams gather in the field to discuss their deployments. ©WHO
The Africa RRT coordinates closely with the ‘virtual’ polio Outbreak Preparedness and Rapid Response Teams (OPRTT), which pulls together additional experts from around the world. In its first year, the RTT ended three cVDPV outbreaks in Kenya, Mozambique and Niger.
The second part of the strategy is the planned roll out of an additional vaccine: the novel oral polio vaccine type 2 (nOPV2). This is a modified version of the existing monovalent oral polio vaccine type 2 (mOPV2) that would be used alongside existing vaccines and outbreak response tools. Clinical trials have shown that nOPV2 provides comparable protection to mOPV2 against poliovirus, while being more genetically stable and therefore less likely to seed new cVDPV2 emergences. nOPV2 could therefore play a key role in eradication, but it is important to remember that the existing polio vaccine remains an effective tool for stopping all forms of polio, as long as all children are immunized.



Outbreak response teams coordinate with nomadic communities to conduct a targeted vaccination campaign in Niger, Lake Chad region following an outbreak of cVDPVs which affected the region in 2017 and 2018. ©️ WHO
The third part of the strategy is focused on strengthening routine immunization, both with bivalent OPV (bOPV), and inactivated polio vaccine (IPV). The more children that are protected – with either vaccine – the quicker cVDPV outbreaks can be stopped. “Whether it is wild poliovirus or cVDPVs, polio spreads like wildfire in places of low immunity,” says Richard Mihigo, Coordinator of the Immunization & Vaccine Development Programme for WHO AFRO. “It requires collective immunity to achieve eradication.”
A health worker prepares a dose of inactivated polio vaccine (IPV) for a child ©️ Andrew Esiebo/WHO
Any break in vaccination activities risks a major setback against polio. A new hurdle in the fight against cVDPVs arose when, in March 2020, measures designed to curb the spread of COVID-19 meant immunization campaigns were temporarily suspended.
The GPEI lifted the recommendation on pausing campaigns in May for the most at-risk countries. In early July, Burkina Faso delivered a four-day mass polio immunization campaign, vaccinating just over 174,000 children under five years of age, while Angola vaccinated nearly 1.2 million children of the same age group. Campaigns will continue in other affected countries in the remainder of 2020.


“The campaigns run by the Polio Eradication Programme demonstrate that mass immunization can be safely conducted under the strict implementation of COVID-19 infection prevention and control guidelines,” said Dr Matshidiso Moeti, WHO Regional Director for Africa.
Africa has successfully stopped transmission of wild poliovirus. Elimination of cVDPVs is all that remains. The final push to rid the continent of all forms of polio will require everyone – from government leaders to civil society and communities – to continue their efforts to reach all children with polio vaccines. With sustained funding and unified commitment, the end is in sight.
Outbreak response teams coordinate with nomadic communities to conduct a targeted vaccination campaign in Niger, Lake Chad region following an outbreak of cVDPVs which affected the region in 2017 and 2018. ©️ WHO
Outbreak response teams coordinate with nomadic communities to conduct a targeted vaccination campaign in Niger, Lake Chad region following an outbreak of cVDPVs which affected the region in 2017 and 2018. ©️ WHO
Outbreak response teams coordinate with nomadic communities to conduct a targeted vaccination campaign in Niger, Lake Chad region following an outbreak of cVDPVs which affected the region in 2017 and 2018. ©️ WHO


